Why I Started Learning About Hormones: My Journey through PCOS and Insulin Resistance
Learn why our pharmacist Linda started learning about insulin resistance and women's hormones from her diagnosis of PCOS
Linda Nghiem, Madeline Crichton (pharmacy student)
2/18/20267 min read
You don't become passionate about something until it affects you personally, whether through a patient, a friend, family member, or yourself. People have wondered why I chose to specialize in menopause and women's hormones.
It all started a few days before my 18th birthday. I was in California visiting family, and I started having severe abdominal pain. Appendicitis? No. Several thousand dollars of hospital bills later, investigations revealed that I had an ovarian cyst. It resolved on its own in a few weeks, and life went on. Fast forward four years: Blood tests showed that I had elevated testosterone levels. I had irregular periods. I had acne and a few facial hairs. Surprisingly to the doctor, I was normal weight. The diagnosis was PCOS: polycystic ovarian syndrome.
The diagnosis did not have much impact on me until years later when we encountered difficulty conceiving. After dealing with the depressed feelings that come with infertility, I finally dug my heels in and did some research. Why is this was happening to me? I have to understand, and take control of my hormones! I am fortunate enough to have the pharmacy educational background to learn, decipher, and start to understand the medical literature involved. Have I unscrambled the jigsaw puzzle of hormones? Absolutely not! However, there are some sections that are starting to appear.
PCOS and Insulin resistance
Specifically for PCOS, we aim to reduce or eliminate insulin resistance through changes in diet, exercise, and medications. Insulin is a hormone in the body which helps regulate blood sugar. Normally when your blood sugar is high (for example after eating a meal) the body will release insulin. Insulin helps muscle, liver, and fat cells to absorb sugar from the blood, providing cells with a source of energy and lowering sugar in the blood. Insulin also stimulates cells to make proteins, fats, and glycogen (storage form of sugar).
Insulin resistance is when the body cannot respond normally to insulin. Insulin resistance generally happens when blood sugar levels are elevated for long periods of time. The body makes more insulin to try and lower blood sugar. However, the cells of the body can’t keep absorbing sugar from the blood. This means the body will produce more insulin, but the cells of the body are not able to keep up with demand, which is known as insulin resistance.
Without treatment (including changes to diet, exercise, or medications), insulin resistance leads to increasing blood sugar over time as the body cannot effectively remove sugar from the blood. The body will also produce more insulin over time. Insulin resistance can also raise triglycerides (a type of fat) in the blood. To identify insulin resistance, your healthcare provider may send you for blood work. These blood tests may include:
A1c: a measure of your average blood sugar over the past 3 months. This is checked by looking at the amount of sugar on your red blood cells, which is affected by your blood sugar
Fasting blood glucose: a measure of blood sugar after not eating for a period of time, usually at least 8 hours.
Insulin: a measure of the how much insulin is in your blood.
Lipid panel: a measure of levels of total cholesterol, LDL, HDL and triglycerides in the blood.
Insulin resistance is also associated with the development of diabetes or heart disease. Other medical conditions such as polycystic ovarian syndrome (PCOS), and metabolic dysfunction associated steatoic liver disease (MASLD, formerly known as non-alcoholic fatty liver disease or NAFLD) are also associated with insulin resistance. Insulin resistance is associated with weight gain, insulin resistance can make it more difficult to lose weight, because insulin promotes fat storage.
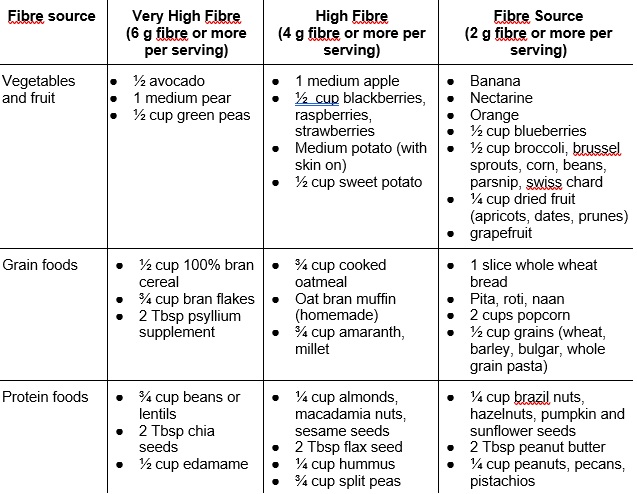
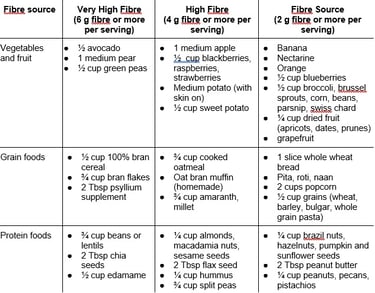
Insulin resistance can be reversed and improved through changes to diet, exercising, and through certain medications. Weight loss is often important for improving insulin resistance. There are many dietary options that can improve insulin resistance. Ideally, the diet should focus on getting a variety of foods. The diet should focus on high fibre intake and include lots of whole grains and fruits and vegetables. A diet for reversing insulin resistance should also limit processed foods, especially those that are high in sugar. Dietary goals include:
Fibre intake of 25 g/day
Eating at least 2 servings of vegetables per day
Eating at least 3 servings of fruit per day
When making dietary changes it is important to work slowly so your body can adapt to reduce bloating and stomach discomfort. For example if you have never eaten lentils before and you want to add them as a source of protein and fibre, you may want to start with 1-2 Tbsp at a meal and increase slowly after a few days. If you are focusing on a goal of eating a fruit and vegetable at every meal you may want to start with 1 meal per day and increase on a steady basis. Making changes slowly helps your body adapt, but also can help with forming habits. It can be overwhelming to change your entire diet all at once, so adding or removing foods slowly may help make changes feel less overwhelming.
Exercises that improve strength (e.g. resistance training, free weights, yoga, pilates) and aerobic exercises (cardio such as walking, jogging, biking and swimming) are important for overall health and improving insulin resistance. Strength training builds muscle mass which is important in insulin resistance because the muscles absorb sugar from the blood. Increasing the amount of muscle you have can increase the amount of sugar absorbed from the blood and used/stored in the muscles. A goal to target is incorporating some sort of strength training into your routine 2 days a week. If you do not currently do any strength training you may want to start with 1 shorter session (eg. 10-15 minutes) per week for a few weeks, and slowly increase. The best strength training is something you enjoy, and could include things like yoga, dancing, lifting weights, body weight exercises like squats or planks, or many other things.
Aerobic exercise or cardio uses energy stores from the muscles and burns fat. The body will replenish stored energy, which will lower blood sugars. A goal to aim for is 150 minutes per week of moderate intensity physical activity. This may look different for different people but may mean 30 minutes of moderate activity 5 days a week. If you do not currently do any aerobic exercise you may want to start slowly with 5-10 minutes per day of walking, or a low impact exercise such as swimming. After you consistently complete this for a few weeks you can increase the quantity of exercise by 5-10 minutes/day. The best aerobic exercise is something you enjoy, and could include biking, walking, jogging, rowing, or swimming.
Several medications improve insulin resistance. Some medications are studied only for specific conditions and may not be appropriate for every patient situation. In PCOS, metformin is used most commonly to improve insulin sensitivity. It can take up to 6 months to restore menstrual cycles and lower testosterone levels. Supplements such as inositol and berberine have been shown to improve insulin sensitivity as well. For diabetes, there are other medications that can improve insulin sensitivity. For the purpose of this blog post, I will not be discussing medications in further detail.
Back to my journey
If you have read my previous blog posts, you already know I am a picky eater and hated vegetables. It took time, but one broccoli floret at a time, I started eating better. Just before the two year mark of trying for a child, we finally conceived our beautiful baby girl. But wait! Not even a year after birthing her, we were expecting another. What happened? I went from infertile to way too fertile! Eek!
My interest in insulin resistance led to become a Certified Diabetes Educator. I continued my lifestyle changes. A couple years later did I notice that my menstrual cycles had completely changed: I had regular monthly cycles, had little to no menstrual cramping, and had less blood loss each month. No more acne. Contraception was necessary. Mood changes were not welcome, but were predictable, depending on the time of the month. What a difference from my younger years! But what is to come...?
I wanted to find out more about hormones because of my earlier experience with PCOS and infertility. Many patients were asking about their experience with perimenopause. I needed answers about women's sex hormones. Women experience these hormone fluctuations monthly, leading to (at times) a roller coaster of emotions, weight, breast size and sexual desire. Extreme changes in hormones in women are marked by the rise in hormones at puberty, the drop of hormones before/at menopause, and for some women, a peak during pregnancy and the following trough in the post-partum phase. To better understand women's sex hormones and their effects, I better educated myself through the menopause guidelines leading to my certification with the Menopause Society. Many people can say they are an expert in hormones, and there are many bold claims made on the internet, often without supporting evidence. There are many aspects of hormones that we have yet to understand, as the network of hormones is complicated by many factors. Unfortunately, there have been poorly designed and poor quality (i.e. BAD) studies that have made the landscape confusing and simply scary to delve into. Fortunately, there is more interest and research to come. What I want you to know is:
Your lifestyle affects your hormones.
It is estimated that there are more than 200 hormones in our body, having effects on our bodily functions, metabolism, mood, and fertility. Commonly known hormones include insulin, thyroid hormones, cortisol, estrogen, progesterone, and testosterone. Hormone levels can change the type of diet that you eat long term, such as whether you eat a high-fat diet, low-carb diet, plant-based diet, North American diet, Mediterranean diet or if you calorie restrict. I am one person who chose to eat more fruits and vegetables and less processed food. I can say confidently that I no longer have PCOS. Mentally and physically, I feel better and in control in my life. I encourage these lifestyle changes to reduce the risk of chronic conditions like cardiovascular disease, diabetes and dementia, and to improve quality of life.


Monday - Thursday: 9:00 AM to 5:30 PM
Friday: 9:00 AM to 5:00 PM
Saturday: 10:00 AM to 2:00 PM
© 2025. All rights reserved.
